Jason Prestinario is CEO of Particle Health. The company is best known for its current lawsuit against Epic, but behind that there is a real company delivering a set of products as on ramp for clients wanting to access health data. Particle was cut off from access to Carequality & Epic a couple of years back but is now both delivering services to its customers and separately suing Epic for being an abusive monopoly regarding its payer platform. I had written about this a couple of years ago but I used this chance to catch up with Jason, to see what the sate of play was. He explained that Carequality said that Particle was right in the original dispute, and why they were right and Epic was wrong. The court case continues. But it’s interesting to hear from someone in the middle of the new disputes about data. — Matthew Holt
Assault on Scientific Integrity Is “Fundamentally Problematic.”

By MIKE MAGEE
This past week, U.S. District Court Judge Judge Brian E. Murphy, dealt Trump and RFK Jr. a severe blow. Not mincing word, he voided HHS vaccine schedule changes and labeled the action an assault on scientific integrity that was “fundamentally problematic.”
In early December, 2025, President Trump directed HHS Secretary Robert Kennedy to review the standing childhood immunization schedule. That schedule has historically guided the state school-entry requirements for vaccines as well as mandating no out-of-pocket costs to parents from vaccine insurers.
The order had followed Kennedy’s summary dismissal of all members of the CDC’s Advisory Committee on Immunization Practices replacing them with a suspect group of vaccine skeptics without any peer review.
Professional organizations, including the American Academy of Pediatrics and the American Medical Association quickly challenged the action in court.
Judge Murphy suspended the appointment of 13 of the 15 new vaccine panel members, and stated that only 6 of the 125 “even under the most generous reading, have any meaningful experience in vaccines.” The swift rebuke followed the evaluation of the new RFK Jr. appointed group’s work output by an independent coalition of scientific researchers which documented 60 misleading or false segments and vaccine claims in their inaugural December meeting.
AAP President Andrew Racine M.D. was quick to applaud the court’s decision, stating ““This decision effectively means that a science-based process for developing immunization recommendations is not to be trifled with and represents a critical step to restoring scientific decision-making to federal vaccine policy that has kept children healthy for years.”
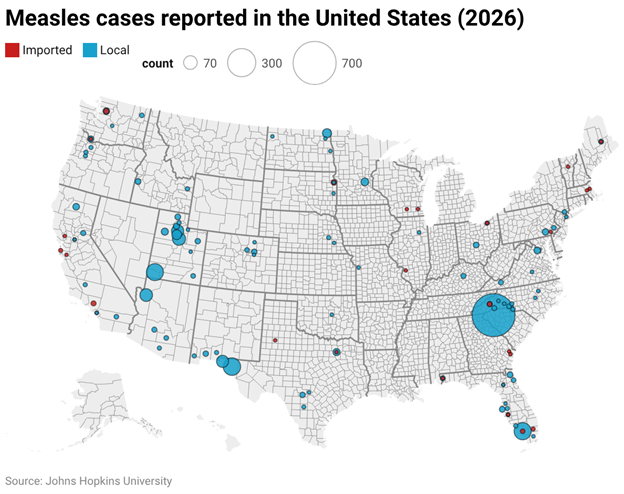
The action couldn’t come soon enough according to state Public Health officials across the country who have been struggling to turn around a Measles epidemic tied to lax vaccination rates.
Continue reading…Mario Danek, QNovia
Mario Danek is CEO of QNovia, a behavior change platform focusing on smoking cessation product. Essentially the problem with smoking cessation nicotine products is that they don’t deliver the “hit” of a cigarette as quickly as a cigarette or a vape. Mario’s new vape-like product delivers a nicotine replacement therapy (think like Nicorette gum) just as quickly as the form factor it’s replacing. He is hoping that the device/drug/and forthcoming mental health support will be the engine to reduce the current smoking rate from the stubborn level it’s got stuck at. He told me about its likely time to commercialization–Matthew Holt
Beyond Generative AI

By BENJAMIN EASTON
Healthcare’s administrative burden is not a documentation problem. It is a workflow problem. Healthcare’s next leap depends on agentic systems that can actually do the work
Over the past year, healthcare organizations have widely adopted generative AI for an array of documentation-related activities such as drafting appeal letters, producing patient-friendly summaries, and even assisting with administrative writing. While these tools have improved how information is created, healthcare’s administrative bottlenecks (e.g., prior authorizations, benefit verification, denial management, clinical trial enrollment), are not caused by a lack of text. They are caused by fragmented systems, manual tracking, payer variability, and workflow handoffs that require continuous monitoring and intervention.
If generative AI helps write the email, agentic systems send it, track it, escalate it, reconcile the response, and close the loop.
That distinction is healthcare’s next inflection point.
From Content Generation to Workflow Execution
An agentic system is not just a chatbot layered onto healthcare workflows. It is a coordinated set of AI-driven agents designed to:
- Pull structured and unstructured data from EHRs, payer portals, labs, and internal systems
- Apply payer-specific policy logic
- Validate documentation requirements
- Submit transactions through the appropriate channel
- Monitor status changes
- Trigger follow-up actions
- Escalate exceptions to humans
- Log every action for audit and compliance
Behind the scenes, these systems rely on rule engines, structured clinical mappings, secure API integrations, and event-driven automation frameworks. They continuously re-evaluate state changes (e.g., a new lab result, a status update from a payer portal, or a missing documentation flag) and dynamically adjust next steps.
This is not robotic process automation replaying keystrokes. It is intelligent orchestration across disconnected systems.
Continue reading…Preeti Bhargava, Arintra
Preeti Bhargava is CTO of Arintra. She is the living embodiment of my crack that the smartest people in the world spent the 2010s convincing people to click on ads and now spend their time figuring out how to bill payers more for providers doing the same work. Arintra is in the RCM business. It uses AI to read the medical chart and automatically generate claims using fewer human coders, and generating up to a 5% revenue uplift for one customer, Mercy Health. Of course those paying those claims may have noticed, so we had a chat about the emerging AI RCM arms race–Matthew Holt
How Digital Narratives Shape Mental Health Outcomes

By SUHANA MISHRA
When discussing treatment outcomes, we usually talk about dosage, adherence, and access. Rarely do we speak about algorithms.
Yet as I began working on a scoping review examining misinformation and disinformation in mental health with a team at the Royal College of Psychiatrists led by Dr. Subodh Dave, I realized that some of the most powerful determinants of patient outcomes are not confined to clinics. They live in comment sections, short-form videos, and anonymous threads that shape people’s view on what is the “truth”. In fact, the NY Post says, “over half of top TikTok mental health videos contained misleading information”.
I chose to do this research because I’ve seen how a single online post or video can change the way someone thinks about their own mental health. I’ve witnessed my very own family members be discouraged to follow a treatment plan based on an inaccurate post sent in a WhatsApp group chat. By examining misinformation in collaboration with experts, I hope to identify practical strategies to help clinicians and public health professionals address their hidden determinants of mental health outcomes.
One of the most striking lessons that I’ve learned is that misinformation in psychiatry doesn’t always seem like a conspiracy. It can often seem like comfort. According to an ArXiv study from Cornell University, people adopt misinformation because it satisfies psychological and social needs rather than accuracy goals.
A viral post on a Reddit thread r/antipsychiatry which claimed antidepressants “numb your personality” may be rooted in one person’s difficult experience. A video on tiktok circulating discouraging medication in favor of “natural rewiring” may promise autonomy in a system that feels impersonal. These narratives spread not because they are outrageous conspiracy theories, but because they really resonate with people.
That resonance has consequences.
Continue reading…Oscar-Nominated Film Highlights Shared American, Iranian Health System Concerns

By MICHAEL MILLENSON
At the recent Academy Awards broadcast, a brief film clip from the Oscar-nominated Iranian film “It Was Just An Accident” showed a man pushing an unconscious, very pregnant woman on a gurney into a hospital emergency room. Without intending to do so, the excerpt pointed to one of the many common concerns shared by Iranians and Americans when dealing with their respective health care systems.
In the Iranian movie, a hospital desk clerk turns away the woman for lack of a payment up front with cash or a credit card. Although that kind of rejection is supposed to be illegal in America, indigent patients can be turned away if the hospital simply tells them their problem isn’t urgent. Even if accepted as self-pay, they might find themselves being billed up to 13 times what the hospital accepts from the government.
Yet it’s not just high costs and unfeeling bureaucrats that worry both Americans and Iranians – although Oscars host Conan O’Brien did joke that in the movie “Hamnet,” Shakespeare’s wife giving birth alone in the woods was “what we call in America ‘affordable health care.’” Iran is an urbanized nation of 93 million people. While the radical hostility to Western values of its clerical rulers is an important contributor to the current war with America, the society as a whole struggles with many of the same health-system problems as other developed countries, including the United States, and often approaches them in a similar way. Still, there are some exceptions unique to the Iranian context.
Consider Iranian researchers articles about diabetics’ experiences at the doctor’s office; ensuring a future supply of nurses; and health insurance utilization and expenditures for a particularly vulnerable population. Though all are topics which might equally appear in a U.S. journal, what sets them apart here is the authorship. At least one co-author of each is affiliated with an institution whose origins would seem as far away from health services research as imaginable. That’s Teheran’s Baqiyattalah University of Medical Sciences, (pictured below) which was founded by the Islamic Revolutionary Guard Corps.

Affiliation aside, Iranian researchers are typically trained much like their U.S. counterparts, and that’s reflected in both their work and the international journals where it’s published.
Continue reading…Stuck in the Middle

By KIM BELLARD
Even before the war – oops: special operation, excursion, or whatever your preferred term is – with Iran started, people were complaining about how expensive things are. Home ownership for first time buyers seems out of reach. Sure, egg prices may be down from the late stages of the Biden Administration (thank you so much, bird flu!), but most of us are still dismayed by our grocery bills. Health insurance costs what a house might have cost fifty years ago and what a new car might have cost twenty years ago.
The latest findings from the West Health-Gallup Center on Healthcare in America show that a third of Americans have cut back on expenses in order to pay health care expenses. We’re stringing out their prescriptions, borrowing money, even skipping meals to pay our health care bills. Even among those with health insurance 29% are cutting back; 62% of those without health insurance are making trade-offs, and I’m surprised the latter isn’t much higher.
Similarly, Kaiser Family Foundation found that 4 in 10 Americans have not taken their prescription medications due to costs, and 6 in 10 worry about being able to afford prescription drugs for themselves or their families. Even among those with insurance, a majority worry.
Gallup also found that Americans are delaying major life events due to their health care costs, including taking vacations (29%), surgical or medical treatments (26%), or changing jobs (18%). Even a quarter of those with family incomes over $240,000 report such delays.
Continue reading…Jesse Shoplock, Inbox Health
Jesse Shoplock is SVP of Business Development at Inbox Health. They are trying to help one of the messiest parts of American health care, figuring out both how much patients owe at the point of care and how to actually help the providers get paid. As of now 70% of patients don’t know what they owe, and in some cases those patients payments are 30% of total revenue and a bug chunk of that isn’t being collected. Jess told me how they are helping practices fix that. (And in the answer to my question Jesse didn’t know, they’ve raised some $55m so far)–Matthew Holt
Ratnakar Lavu, Elevance
Ratnakar Lavu is the Chief Digital Information Officer of Elevance, the holding company of Blue Cross and Blue Shield plans in some 14 states (usually called Anthem Blue Cross). We had a great chat about what the priorities are for Elevance, and Ratnakar’s goal is to use tech to make the member experience simple. They are leaning heavily on AI and chatbots to help members inform themselves, and to help providers speed up approvals for prior auth et al. We also discussed how they work with vendors and how they help them scale.–Matthew Holt









