Berenson, Pronovost & Krumholz
 There is a consensus that measuring performance can be instrumental in improving value in U.S. health care. In particular clinical areas, such as cardiac and intensive care, measurement has been associated with important improvements in providers’ use of evidence-based strategies and patients’ health outcomes over the past two decades. Perhaps most important, measures have altered the culture of health care delivery for the better, with a growing acceptance that clinical practice can and should be objectively assessed.
There is a consensus that measuring performance can be instrumental in improving value in U.S. health care. In particular clinical areas, such as cardiac and intensive care, measurement has been associated with important improvements in providers’ use of evidence-based strategies and patients’ health outcomes over the past two decades. Perhaps most important, measures have altered the culture of health care delivery for the better, with a growing acceptance that clinical practice can and should be objectively assessed.
Nevertheless, as we argue in the full-length version of this paper, substantial shortcomings in the quality of U.S. health care persist. Furthermore, the growth of performance measurement has been accompanied by increasing concerns about the scientific rigor, transparency, and limitations of available measure sets, and how measures should be used to provide proper incentives to improve performance.
The challenge is to recognize current limitations in how measures are used in order to build a much stronger infrastructure to support the goals of increased accountability, more informed patient choice, and quality improvement. In the following paper, we offer seven policy recommendations for achieving the potential of performance measurement.
1. Decisively move from measuring processes to outcomes.
There is growing interest in relying more on outcome measures and less on process measures, since outcome measures better reflect what patients and providers are interested in. Yet establishing valid outcome measures poses substantial challenges—including the need to riskadjust results to account for patients’ baseline health status and risk factors, assure data validity, recognize surveillance bias, and use sufficiently large sample sizes to permit correct inferences about performance.
Read more.
2. Use quality measures strategically, adopting other quality improvement approaches where measures fall short.
While working to develop a broad set of outcome measures that can be the basis for attaining the goals of public accountability and information for consumer choice, Medicare should ensure that the use of performance measures supports quality improvement efforts to address important deficiencies in how care is provided, not only to Medicare beneficiaries but to all Americans. CMS’ current focus on reducing preventable rehospitalizations within 30 days of discharge represents a timely, strategic use of performance measurement to address an evident problem where there are demonstrated approaches to achieve successful improvement [6]. Read more.
Continue reading…
 The first time I met one of my staff physicians on Internal Medicine, he told our team he had just one rule:
The first time I met one of my staff physicians on Internal Medicine, he told our team he had just one rule:
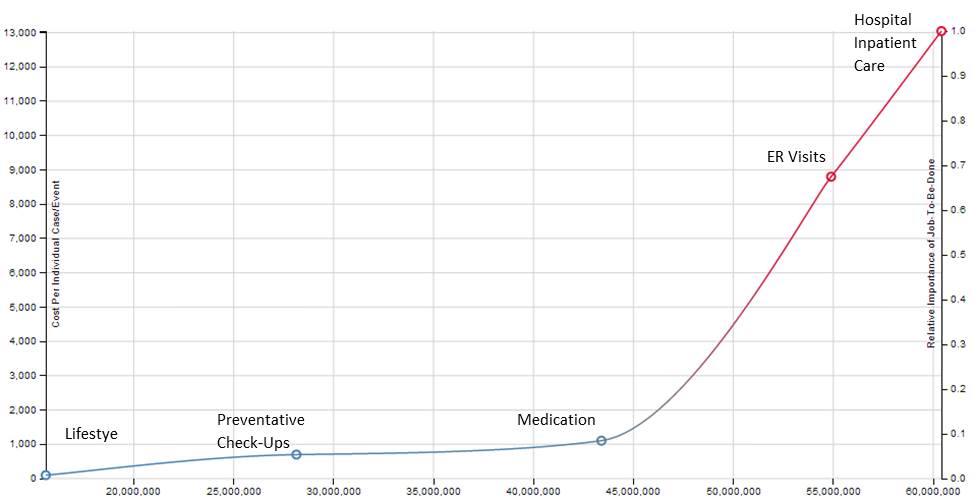


 Patients, payers, policy-makers, and providers all care about the end results of care—not the technical approaches that providers may adopt to achieve desired outcomes, and may well vary across different organizations. Public reporting and rewards for outcomes rather than processes of care should cause provider organizations to engage in broader approaches to quality improvement activities, ideally relying on rapid-learning through root cause analysis and teamwork rather than taking on a few conveniently available process measures that are actionable but often explain little of the variation in outcomes that exemplifies U.S. health care.
Patients, payers, policy-makers, and providers all care about the end results of care—not the technical approaches that providers may adopt to achieve desired outcomes, and may well vary across different organizations. Public reporting and rewards for outcomes rather than processes of care should cause provider organizations to engage in broader approaches to quality improvement activities, ideally relying on rapid-learning through root cause analysis and teamwork rather than taking on a few conveniently available process measures that are actionable but often explain little of the variation in outcomes that exemplifies U.S. health care.






