 The aging of populations worldwide is leading to many healthcare challenges, such as an increase in dementia patients. One recent estimate suggests that 13.9% of people above age 70 currently suffer from some form of dementia like Alzheimer’s or dementia associated with Parkinson’s disease. The Alzheimer’s Association predicts that by 2050, 135 million people globally will suffer from Alzheimer’s disease.
The aging of populations worldwide is leading to many healthcare challenges, such as an increase in dementia patients. One recent estimate suggests that 13.9% of people above age 70 currently suffer from some form of dementia like Alzheimer’s or dementia associated with Parkinson’s disease. The Alzheimer’s Association predicts that by 2050, 135 million people globally will suffer from Alzheimer’s disease.
While these are daunting numbers, some forms of cognitive diseases can be slowed if caught early enough. The key is early detection. In a recent study, my colleague and I found that machine learning can offer significantly better tools for early detection than what is traditionally used by physicians.
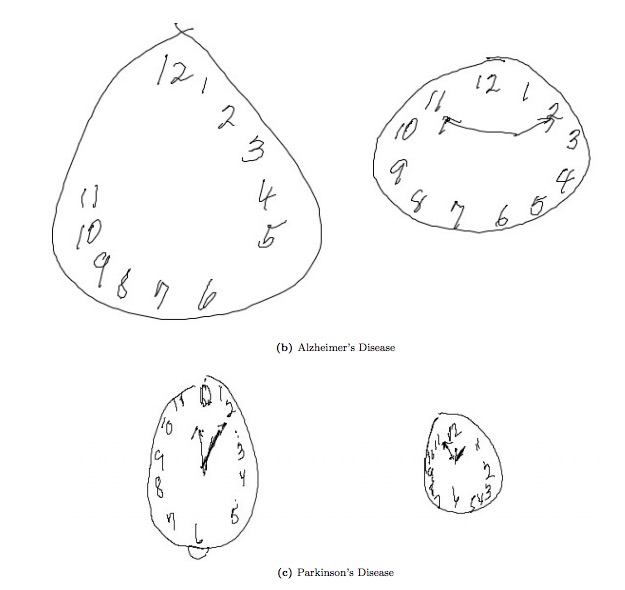
One of the more common traditional methods for screening and diagnosing cognitive decline is called the Clock Drawing Test. Used for over 50 years, this well-accepted tool asks subjects to draw a clock on a blank sheet of paper showing a specified time. Then they are asked to copy a pre-drawn clock showing that time. This paper and pencil test is quick and easy to administer, noninvasive, and inexpensive. However, the results are based on the subjective judgment of clinicians who score the tests. For instance, doctors must determine whether the clock circle has “only minor distortion” and whether the hour hand is “clearly shorter” than the minute hand.
In our study, we created an improved version of this test using big data and machine learning. For the past seven years, a group of neuropsychologists have had patients use a digital pen to draw the clocks instead of a pencil, accumulating more than 3,400 tests in that time. The pen functions as an ordinary ballpoint, but it also records its position on the page with considerable spatial and temporal accuracy. We applied machine learning algorithms to this body of data, constructing a data-driven diagnostic tool. So rather than having doctors subjectively analyze the pencil-drawn clocks, the data from the digital pen drawings goes into the machine learning algorithm’s model which provides the result of the test.
The performance of the model was tested on two tasks – screening (binary classification between healthy and a specific impairment) and diagnosis (selecting the most likely impairment) – on a set of three diagnoses: memory disorders (including Alzheimer’s disease), vascular cognitive dementias, and Parkinson’s disease. The model proved to be more accurate than the traditional Clock Drawing Test scoring systems for both screening and diagnosis, for all three disease. Its results were substantially better than what was reported in the literature for the doctors’ subjective results. On a scale from 0 to 100, physicians’ results with the traditional test were within the range of 66-79 points, whereas the machine learning version scored 89-93 points.
Some of the machine learning models we developed are interpretable; they are constructed using concepts familiar to healthcare providers, enabling them to explain the result to patients.
This is a great example of how machine learning and big data can be used to address important healthcare issues. Our work has the potential to make significant improvements in the screening and possible diagnosis of cognitive decline. While our models require additional testing for validation, they appear to allow for faster results, more accessible and accurate screening, and more reliable diagnoses.
Cynthia Rudin is an associate professor at MIT Sloan School of Management and the MIT Computer Science and Artificial Intelligence Laboratory (CSAIL).
The following researchers contributed to this report: William Souillard-Mandar, Randall Davis, Cynthia Rudin, Rhoda Au, David J. Libon, Rodney Swenson, Catherine C. Price, Melissa Lamar, Dana L. Penney. Learning Classification Models of Cognitive Conditions from Subtle Behaviors in the Digital Clock Drawing Test. Accepted with Minor Revision to Machine Learning, 2015.
Categories: Uncategorized









One of the big differential diagnoses of dementia in older folks is delirium. Think of delirium as intense confusion. Almost anything stressful in someone older than about 75 can start delirium and this can fool us into thinking dementia. A urinary tract infection, a fall, a tooth pulpitis… little things can do it. I wonder how the clock drawing exercise would perform here?
Delirium can usually be reversed and we shouldnt begin treatment for dementia until we have excluded this diagnosis.