The thing to do in health tech this week? Trademark infringement. Today on Health in 2 Point 00, we try to make sense of all the lawsuits right now with Teladoc suing Amwell, Allscripts suing CarePortMD, and whose side are we on for Zocdoc suing Zocdoc? On Episode 160, Jess asks me to make sense of Augmedix’s faux IPO in a reverse merger and publicly traded company Newtopia arising $7 million. Twentyeight Health raises $5.1 million in a Series C and TestCard raises $5.8 million for at-home mobile urine testing. —Matthew Holt
THCB Spotlights: Jon Bloom, Podimetrics
By MATTHEW HOLT
This is a fun conversation with Jon Bloom, the CEO of Podimetrics. It’s one of a number of competitors trying to help prevent foot ulcers among people with diabetes. Some use socks, others use insoles, but Podimetrics’ approach is to use a SmartMat which looks like a weight scale and can tell whether a patient might be developing a foot ulcer and is therefore at risk for amputation. Last week Podimetrics and Kaiser Permanente released a study that showed SmartMat and wraparound/care management service showed great success in reducing hospitalization, ER visits and foot amputations. But Bloom thinks that there’s much more to the care of very sick & underprivileged people with diabetes, and we had a great discussion about that that might look like.
Tying Health Care Investment to Performance
By BRIAN KLEPPER and JEFFREY HOGAN


GoodRx’s planned initial public offering recently made the news, notable because the company, launched in 2011, has been profitable since 2016. Evidently, it’s become unfashionable for investors to demand proof of performance, so GoodRx’s results shone like a beacon. By contrast, most health care firms seeking funding convey bold aspirations and earnest promises. Investors throw in with them and hope for the best.
But few new entrants seem to do the necessary advanced due diligence to assess exactly where and how their product, service or innovation should be positioned in the health care ecosystem to derive maximum value. Ironically, COVID has intensified and highlighted the fragility of the health care ecosystem, as well as the greater disruption opportunities available to new entrants.
Health care has become irresistible to investors, the outgrowth of the industry’s dominant players’ spectacular financial performance. Over the past 45 quarters, for example, major health plan stock prices have grown 4-6 percent per quarter, 1.2-2.2 times the growth rates of DJI and S&P (See the table below). Investors hope to either 1) capitalize on the health care’s ongoing culture of overtreatment and egregious pricing, or 2) support and share in the savings associated with rightsizing care and cost.
Continue reading…Will Trump, Congressional Infections Boost Innovations For Covid-19 Survivors?

By MICHAEL MILLENSON
When powerful politicians confront a life-threatening diagnosis, it can change policy priorities.
In addition to President Trump and a slew of top aides, five U.S. senators and 15 members of the House of Representatives have now tested positive or been presumed positive in tests for Covid-19 as of Oct. 5, according to a running tally by National Public Radio (NPR).
In that light, the recent burst of coronavirus infections could accelerate three significant innovations affecting every Covid-19 survivor.
1) Post-Covid Clinics
Even seemingly mild encounters with the coronavirus can trigger a cascade of lingering health consequences. While “there is no consensus definition of post-acute Covid-19,” noted an Oct. 5 JAMA commentary, symptoms that have been reported include joint pain, chest pain, fatigue, labored breathing and organ dysfunction “involving primarily the heart, lungs and brain.”
A survey by Survivor Corps, a patient support group, and the Indiana University School of Medicine found that Covid “long haulers” often suffer from “painful symptoms…that some physicians are unable or unwilling to help patients manage.” A similar survey by the Body Politic Covid-19 Support Group concluded that Covid long-haulers face “stigma and lack of understanding [that] compromise access to health care and quality of support.”
Continue reading…THCB Gang Episode 28 10/15

Episode 28 of “The THCB Gang” was live-streamed on Thursday, October 15th! Watch it below!
Matthew Holt (@boltyboy) was joined by some of our regulars: communications leader Jennifer Benz (@jenbenz), data privacy expert Deven McGraw (@healthprivacy), CEO of addiction recovery service Suntra Modern Recovery, Jean-Luc Neptune MD (@jeanlucneptune), CEO of Day Health Strategies Rosemarie Day (@Rosemarie_Day1), medical historian & health economist Mike Magee MD (@drmikemagee), policy & tech expert Vince Kuraitis (@VinceKuraitis). The conversation focused on the looming election, the new COVID-19 Surge, Amy Coney Barrett’s hearing, and health care costs rising in the US costs.
If you’d rather listen to the episode, the audio is preserved as a weekly podcast available on our iTunes & Spotify channels — Zoya Khan, producer
A War on Science is a War on Us
By KIM BELLARD

We’re in the midst of a major U.S. election, as well as hearings on a Supreme Court vacancy, so people are thinking about litmus tests and single issue voters – the most typical of which is whether someone is “pro-life” or “pro-choice.” Well, I’m a single issue person too; my litmus test is whether someone believes in evolution.
I’m pro-science, and these are scary times.
Within the last week there have been editorials in Scientific American, The New England Journal of Medicine, and Nature – all respected, normally nonpartisan, scientific publications – taking the current Administration to task for its coronavirus response. Each, in its own way, accuses the Administration of letting politics, not science, drive its response.
SA urges voters to “think about voting to protect science instead of destroying it.” They cite, among other examples, Columbia Law School’s Silencing Science Tracker, which “tracks government attempts to restrict or prohibit scientific research, education or discussion, or the publication or use of scientific information, since the November 2016 election.” Their count is over 450 by now, across a broad range of topics in numerous federal agencies on a variety of topics.
The SA authors declare:
Science, built on facts and evidence-based analysis, is fundamental to a safe and fair America. Upholding science is not a Democratic or Republican issue.
Similarly, NEJM fears:
Our current leaders have undercut trust in science and in government,4 causing damage that will certainly outlast them. Instead of relying on expertise, the administration has turned to uninformed “opinion leaders” and charlatans who obscure the truth and facilitate the promulgation of outright lies.
Jeff Tollefson, in Nature, warns:
As he seeks re-election on 3 November, Trump’s actions in the face of COVID-19 are just one example of the damage he has inflicted on science and its institutions over the past four years, with repercussions for lives and livelihoods.
Continue reading…#Healthin2Point00, Episode 159 | A quiet period?
Today on Health in 2 Point 00, we might be seeing a quiet period in health tech investing with the election coming up. On Episode 159, Jess and I talk about TigerConnect raising $45 million in a Series D, offering a HIPAA-compliant texting service for doctors; UK-based startup Numan getting £10 million, which is another online male health clinic. Next, Nym gets $16.5 million—lots of good investors in this round, this company uses natural language processing to automate hospital billing. Finally, Press Ganey acquires Doctor.com and a company called Binary Fountain. —Matthew Holt
#Healthin2Point00, Episode 158 | Datavant, Mira, Avail & more
On Episode 158 of Health in 2 Point 00, Jess and I talk about Datavant raising $40 million in a Series B for their open health data exchange platform, Mira raising $2.7 million for it’s Costco-esque health insurance alternative, Avail raising $100 million providing telehealth for the OR, ScriptDrop raising $15 million for prescription drug delivery, and Abridge raising $15 million to help patients transcribe doctor’s appointments. —Matthew Holt
Health Professionals Are Tomorrow’s Health Journalists. Here is a Code of Ethics to Guide Us and Trump’s White House Doctor.
By MIKE MAGEE

The patient/health-professional relationship is fundamentally grounded in science and trust, and involves the exchange of compassion, understanding and partnership. The Covid-19 pandemic has challenged this relationship by acutely increasing the nation’s burden of disease, creating new barriers to face-to-face contact, and injecting high levels of fear and misinformation.
Dr. Sean Conley, Trump’s White House physician, in his dodgy and evasive management of legitimate questions from the White House press corps regarding the President’s health, has made matters worse.
As this week’s report on an analysis of 38 million articles on the pandemic revealed, much of the misinformation our citizens have experienced can be traced to a single individual who lacks any health credentials – our own President Trump. Sarah Evanega, the director of the Cornell Alliance for Science and lead author of the report stated, “The biggest surprise was that the president of the United States was the single largest driver of misinformation around Covid. That’s concerning in that there are real-world dire health implications.”
The solution to that specific problem is only one month away – vote him out. But if Trump can be successfully sent packing, how prepared are our health professionals, in the face of these new and complex challenges? A President Biden health reform package will likely include expansion of health care teams, exponential growth of telemedicine, and increasing dependence on reliable information to advance personal health planning.
Today’s modern health professionals are tomorrow’s health journalists. What principles should guide them in their new and expanded role. As a guide, I offer the following:
Continue reading…Value-based care – no progress since 1997?

Humana is out with a report saying that its Medicare Advantage members who are covered by value-based care (VBC) arrangements do better and cost less than either their Medicare Advantage members who aren’t or people in regular Medicare FFS. To us wonks this is motherhood, apple pie, etc, particularly as proportionately Humana is the insurer that relies the most on Medicare Advantage for its business and has one of the larger publicity machines behind its innovation group. Not to mention Humana has decent slugs of ownership of at-home doctors group Heal and the now publicly-traded capitated medical group Oak Street Health.
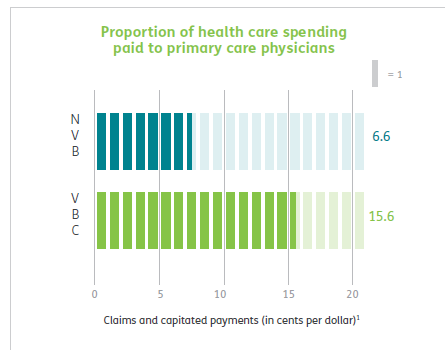
Humana has 4m Medicare advantage members with ~2/3rds of those in value-based care arrangements. The report has lots of data about how Humana makes everything better for those Medicare Advantage members and how VBC shows slightly better outcomes at a lower cost. But that wasn’t really what caught my eye. What did was their chart about how they pay their physicians/medical group

What it says on the surface is that of their Medicare Advantage members, 67% are in VBC arrangements. But that covers a wide range of different payment schemes. The 67% VBC schemes include:
- Global capitation for everything 19%
- Global cap for everything but not drugs 5%
- FFS + care coordination payment + some shared savings 7%
- FFS + some share savings 36%
- FFS + some bonus 19%
- FFS only 14%
What Humana doesn’t say is how much risk the middle group is at. Those are the 7% of PCP groups being paid “FFS + care coordination payment + some shared savings” and the 36% getting “FFS + some share savings.” My guess is not much. So they could have been put in the non-VBC group. But the interesting thing is the results.