
By MIKE MAGEE
This past week, U.S. District Court Judge Judge Brian E. Murphy, dealt Trump and RFK Jr. a severe blow. Not mincing word, he voided HHS vaccine schedule changes and labeled the action an assault on scientific integrity that was “fundamentally problematic.”
In early December, 2025, President Trump directed HHS Secretary Robert Kennedy to review the standing childhood immunization schedule. That schedule has historically guided the state school-entry requirements for vaccines as well as mandating no out-of-pocket costs to parents from vaccine insurers.
The order had followed Kennedy’s summary dismissal of all members of the CDC’s Advisory Committee on Immunization Practices replacing them with a suspect group of vaccine skeptics without any peer review.
Professional organizations, including the American Academy of Pediatrics and the American Medical Association quickly challenged the action in court.
Judge Murphy suspended the appointment of 13 of the 15 new vaccine panel members, and stated that only 6 of the 125 “even under the most generous reading, have any meaningful experience in vaccines.” The swift rebuke followed the evaluation of the new RFK Jr. appointed group’s work output by an independent coalition of scientific researchers which documented 60 misleading or false segments and vaccine claims in their inaugural December meeting.
AAP President Andrew Racine M.D. was quick to applaud the court’s decision, stating ““This decision effectively means that a science-based process for developing immunization recommendations is not to be trifled with and represents a critical step to restoring scientific decision-making to federal vaccine policy that has kept children healthy for years.”
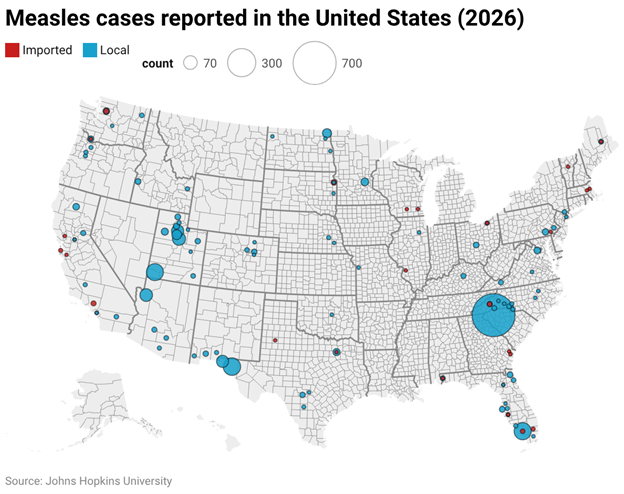
The action couldn’t come soon enough according to state Public Health officials across the country who have been struggling to turn around a Measles epidemic tied to lax vaccination rates.
Continue reading…













